The relationship between mental and physical illness has always been one of the most fascinating—and vexing—subjects of medical inquiry. How do physical changes translate into changes of behavioral or cognitive symptoms? How do mental and emotional states affect physiology?
The condition known as Pediatric Autoimmune Neuropsychiatric Disorders Associated with Streptococcal Infections (PANDAS), and the related disorder called Pediatric Autoimmune Neuropsychiatric Disorders (PANS), dwell precisely at that crossroad of psyche and soma.
More than 20 years since it was first described, PANDAS remains controversial and it is still raising important clinical and research questions.
The recent emergence of a new diagnostic test panel has potential to deepen that dialog by providing biological evidence for the autoimmune process thought to trigger the neuromotor symtoms observed in patients that fit the PANDAS/PANS description. Hopefully, it will also lead to better treatment.
 A 20-Year Controversy
A 20-Year Controversy
Two decades ago, Dr. Susan Swedo and her team in the Section of Behavioral Pediatrics at the National Institute of Mental Health (NIMH) first identified a new subtype of pediatric Obsessive Compulsive Disorder (OCD).
The hallmark of this proposed disorder was the sudden acute onset of debilitating anxiety and mood lability accompanied by obsessive/compulsive behavior and/or tics following some sort of strep-associated infection, typically strep throat. The symptoms seemed to be triggered by cross-reactive antibodies produced in response to Group A beta-hemolytic streptococci.
In a landmark 1998 paper, they described the first 50 cases, and named the condition “PANDAS” (Swedo SE, et al. Am J Psychiatry. 1998: 155 (2): 264-71).
In 2008, Lombroso and Scahill proposed five diagnostic criteria for PANDAS: (1) the presence of a tic disorder and/or OCD consistent with DSM-IV; (2) prepubertal onset of neuropsychiatric symptoms; (3) a history of a sudden onset of symptoms and/or an episodic course with abrupt symptom exacerbation interspersed with periods of partial or complete remission; (4) evidence of a temporal association between onset or exacerbation of symptoms and a prior streptococcal infection; and (5) adventitious movements (e.g., motoric hyperactivity and choreiform movements) during symptom exacerbation (Lombroso PJ, Brain Dev., 2008 Apr, 30(4): 231-237).
Additional cases have been documented in which patients present with all the criteria for PANDAS, but lack any evidence of a preceding strep infection. These types of cases, where strep cannot be reliably linked, the NIMH redefined as Pediatric Autoimmune Neuropsychiatric Disorders (PANS).
An even broader concept, known as Childhood Acute Neuropsychiatric Symptoms (CANS)” was proposed by Dr. Harvey Singer at Johns Hopkins in a 2011 paper (Singer H, The Journal of Pediatrics, 2011, 160:5:725-731).
In 2012 the NIMH established revised criteria and guidelines for PANDAS. These were updated in 2017 by a team including Dr. Swedo, now the Chief of the Pediatric & Developmental Neuroscience Branch.
But the diagnosis remains controversial. Many experts simply do not believe that PANDAS or PANS are true disease entities.
Since Dr. Swedo’s original paper, the criteria have been argued over, written about, and revised. Yet PANDAS has never been formally validated in either the ICD codes or the Diagnostic and Statistical Manual (DSM). While there is supportive evidence suggesting a link between streptococcal infections and aberrations in behavior or cognition, no one has yet provided data showing a definitive causal link.
The hypothesis that strep-induced autoimmune cross-reactivity can drive OCD-like symptoms is compelling and reasonable. But it remains just that: a hypothesis.
Molecular Mimicry
Madeleine Cunningham, PhD, a professor of microbiology at the University of Oklahoma, has dedicated her life’s work to providing the biological evidence for this psychological manifestations observed in PANDAS/PANS.
She believes PANDAS/PANS has an autoimmune etiology and endorses the prevailing hypothesis of molecular mimicry as the mechanism by which the condition develops.
The proposed mechanism suggests that antigens on the cell walls of streptococci are similar enough to proteins within the heart valve, joints, and brain that when an immune reaction is set off, the immune system ends up causing damage to those tissues.
This phenomenon is well documents in children with rheumatic fever who developed heart disease, arthritis, or Sydenham’s chorea. In PANDAS/PANS, the target of these autoantibodies is believed to be neuronal tissue localized in the basal ganglia.
Dr. Cunningham, who worked with Dr. Swedo at NIH, developed blood assays that help identify anti-neuronal autoantibodies in PANDAS/PANS patients. The Cunningham Panel™ 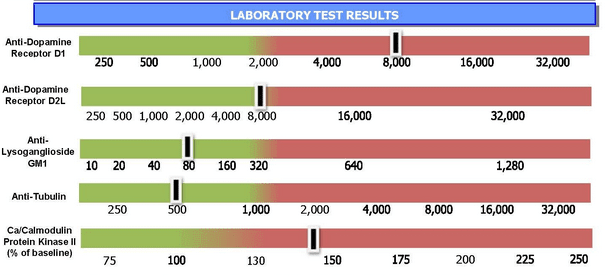 offering by Moleculera Labs is comprised of five different tests. Four are enzyme-linked immunosorbent assays (ELISAs) that measure antibody titers against neuronal antigens present in the brain: Anti-Dopamine Receptor D1, Anti-Dopamine Receptor D2L, Anti-Lysoganglioside GM1, Anti-Tubulin, and Ca/Calmodulin Protein Kinase II.
offering by Moleculera Labs is comprised of five different tests. Four are enzyme-linked immunosorbent assays (ELISAs) that measure antibody titers against neuronal antigens present in the brain: Anti-Dopamine Receptor D1, Anti-Dopamine Receptor D2L, Anti-Lysoganglioside GM1, Anti-Tubulin, and Ca/Calmodulin Protein Kinase II.
If a patient’s Cunningham Panel indicates the presence of abnormally high levels of these antibodies associated with PANDAS/PANS, then it is reasonable to consider a course of steroid therapy. But that needs to be undertaken cautiously. Typically, steroids will reduce the levels of these antibodies present in the blood, which could attenuate the cognitive, behavioral, and motor symptoms.
But this also means that in patients who are currently or recently on steroids, the Cunningham Panel may not return an accurate reading.
If steroid therapy is helpful, but the patient continues to struggle from severe symptoms such as anorexia or suicidal ideation, Dr. Cunningham recommends a trial of plasmapheresis/therapeutic plasma exchange or intravenous immunoglobulin. These are certainly not “first-line” treatment choices, but in many cases they are for promptly resolving symptoms characteristic of PANDAS/PANS.
Dr. Cunningham, who is a co-founder of Moleculera Labs and it’s Chief Science Officer, stresses that antibody testing, and therapies aimed at modulating the immune system, are only part of the story when working with PANDAS patients.
She emphasizes the importance of Cognitive Behavioral Therapy as the first-line of treatment. Learning to cope with the onset of PANDAS/PANS and working to change maladaptive behavioral patterns is fundamental. Selective serotonin reuptake inhibitors are another supportive therapy that has been helpful in reducing the severity of symptoms for some patients.
She also notes that if a patient has an active bacterial infection it is imperative to treat it promptly with antibiotics. That is always the first step.
Testing the Test
As with most other blood tests, the Cunningham Panel must be ordered by a physician registered with a secure Prescriber Portal. At this time, physicians practicing solely in New York State are unable to order the test owing to that state’s unique and restrictive regulations on diagnostic testing.
Though PANDAS and PANS are considered childhood conditions, Moleculera does accept samples from adult patients who have symptoms that meet the PANDAS/PANS criteria, or those who’ve had earlier suggestive histories.
 But keep in mind that Moleculera’s established normal titer ranges for the 5-test panel were determined in normal pediatric populations, so, as of now, there are not any studies supporting the interpretation of the results in adults.
But keep in mind that Moleculera’s established normal titer ranges for the 5-test panel were determined in normal pediatric populations, so, as of now, there are not any studies supporting the interpretation of the results in adults.
The cost of the five tests is $925, of which the patient is expected to submit a deposit of $425 up front. In most cases, Moleculera can bill a patient’s insurance on their behalf. If a patient is uninsured or chooses to file a claim separately, he or she can opt to pay in full. The test does require a blood draw, and the turn-around time is three to four weeks, at which point Moleculera sends the data to the ordering physician via the Prescriber Portal.
While Moleculera is convinced of the relevance and importance of these tests, outside studies have questioned the accuracy of the Cunningham Panel™ in diagnosing PANDAS/PANS.
A Swedish study published in 2017 in the Journal of Immunology found a majority of healthy asymptomatic controls inappropriately received PANDAS diagnoses based on Cunningham Panel test results (Hesselmark E, J Neuroimmunol., 2017 Nov 15; 312:31-37). In other words, these investigators claim the tests generate an unacceptable number of false positives.
Additionally, test-retest reliability proved insufficient. Therefore the researchers concluded they are not supportive of the use clinical use of the Cunningham Panel in diagnosing PANDAS/PANS.
A follow up study published by the same group in 2018 cites a scarcity of well conducted research regarding treatments for PANDAS/PANS and calls for future research to explore potential treatment strategies for these, as well as other variants of OCD with proposed autoimmune etiology (Sigra S, Neurosci Biobehav Rev., 2018 Mar, 86:51-65).
On the lab’s website, Moleculera has issued a statement challenging the conclusions made by the Hesselmark-Bejerot team, noting that these investigators used a type of test tube other than the Glass Red Top tubes required by the lab. The collection tubes used by Hesselmark and colleagues contained a clot activator and a serum gel separator, both of which can interfere with the Cunningham tests.
A clinical consensus regarding optimal treatment strategy is lacking, but the field does agree on one thing: PANDAS/PANS needs more attention. Dr. Cunningham says patient education is one of the most important and proud accomplishments of Moleculera’s efforts.
In the two decades since NIH’s Dr. Swedo and colleagues first named the condition, nobody has been able to roundly dismiss PANDAS/PANS, but the controversy—and the suffering—continues.
If the validity of the Cunningham panel can be firmly established by independent research, it would go a long way toward validating Swedo’s original hypothesis, while also providing a firm and objective way to assess what is currently a vague and difficult diagnosis.
END







