Lyme disease is one of the most vexing conditions challenging physicians today.
The identification of Borrelia burgdorferi, as the primary factor triggering the cascade of pathology we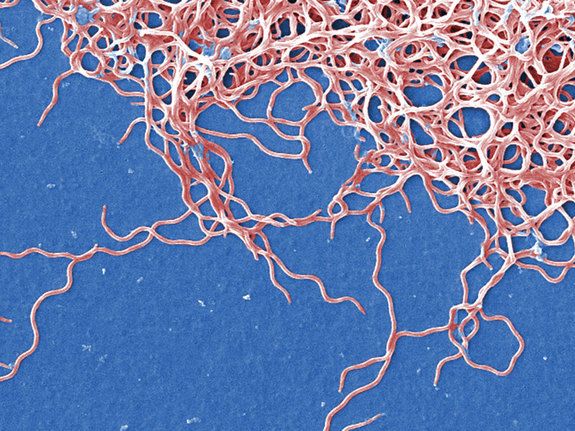 know as Lyme Disease (LD) was a major step forward. But it also over-simplified what turns out to be a much more complicated picture.
know as Lyme Disease (LD) was a major step forward. But it also over-simplified what turns out to be a much more complicated picture.
In addition to Borrelia, several other organisms including Ehrlichia, Babesia, and Rickettsia have also been found associated with the same constellation of symptoms (Alaedini A, Latov N. J Neuroimmunol. 2005; 159:192-195).
One of the key features of LD is the broad impairment of the affected individual’s innate immune response. The usual process of phagocytosis and lysosome recycling does not occur properly (et al., Nature Med, 1999; 5:1375-1382).
The initial exposure to B. bergdorferi renders an individual much more susceptible to assault by other organisms. Chronic infection means that one or more aspects of the immune defense and repair system is persistently impaired.
Impaired Phagocytosis
When phagocytic cells are not able to destroy invasive organisms, these pathogens travel freely through the bloodstream, establish themselves in hospitable tissues, and trigger a number of chronic, sometimes severe symptoms. The initial adaptive response in the skin—the classic erythema multiforme ‘bulls eye’ rash—eventually gives way to joint pain, central nervous system symptoms, and other downstream problems.
Many clinicians these days are making a distinction between LD and the less precise diagnosis of Lyme Syndrome (LS). The latter presents as a multi-system, inflammatory, impaired-repair syndrome.
Neurological and other focal symptoms are due, in part, to deficits of repair capacity in the affected tissues. The following autoimmune, impaired repair syndromes overlap clinically with LS:
- Systemic lupus erythematosis (SLE)
- Thyroiditis
- Multiple Sclerosis (MS)
- Sjogren’s Syndrome
- Rheumatoid Arthritis (RA)
- Diabetes
The variability in the clinical diagnosis of LS has led some to consider it a subjective clinical assessment and not an objectively defined diagnosis.
Be that as it may, it is important to recognize the importance of the underlying immune system impairment, and to realize that phagocytic cells are among the first to run out of ascorbate as well as magnesium, an essential cell electrolyte.
By providing these nutrients in sufficient quantities, we may be able to at least partially reverse the impairment, recharge these first responder cells and possibly prevent further deterioration of health.
Antibiotics are the preferred treatment option for most practitioners working with LD patients. That’s completely appropriate in most cases, but it is important to realize that without improved immune defense and repair functions, the remissions obtained with antibiotics alone will seldom be more than fleeting.
Predictive biomarkers, outlined in this column previously are valuable in helping to determine a given individual’s needs for ascorbate, magnesium and a host of other supplemental nutrients that can support immune system function.
Easing Immune System Burden
Immune memory cells (T and B-lymphocytes) from patients with chronic LD are often reactive not only against Borrelia or other spirochete-specific antigens but also against various host (self) antigens. In a sense, LD gradually transitions from infectious disease to autoimmune disease. This is why it is so difficult to treat.
Like all autoimmune and immune dysfunction conditions, the diagnosis and management of LD is too often empirical, for lack of sufficiently reliable diagnostic and predictive tests. Serology (antibody) studies are particularly misleading because they are unable to distinguish helpful from harmful antibodies.
It is important to identify and eliminate any foods and chemicalsto which a patient is allergic or sensitive. Constant reactions to food allergens or exogenous toxins also take a toll on someone’s immune system and worsen the already significant symptom burden associated with LD itself.
What people eat, drink, think, and do, matter quite a bit when it comes to recovering from LD. As overall health status improves, people become less hospitable to the organisms that trigger LD-associated symptoms. Often, they enter sustained periods of remission and are not susceptible to infection if re-exposed. Technically, they may not be “cured,” but they can live as if they were.
Having gone through the LD journey with several generations of close kin, I have found the following approach to be helpful:
- Reduce Immune Reactions: Detecting true delayed hypersensitivities and substituting effectively for the foods and substances that trigger reactions will unburden the immune system.
- Judicious Use of Supplements: Nutrients can be tailored to each person’s life-style based on predictive biomarkers. Nutrients critical to immune system health include:
Buffered, 100% L-Ascorbate (vitamin C) along with higher bioavailable polyphenolics (quercetin dihydrate and soluble OPC) and CoQ10 with tocopherols micellized in 100% rice bran oil to enhance repair and thus reduce inflammation. Intake should be sufficient to lower the hsCRP value below 0.5 mg/dl.
Glutamine recycled with PAK (pyridoxal ketoglutarate)
Multi-strained probiotic formulation, with fiber to address digestive issues, and to reduce host-hospitality to infection.
Magnesium & Choline citrate: Dosing should be based on first morning urine pH measurements. Magnesium is nature’s calcium channel blocker as well as a protective antioxidant.
- Living better the “Alkaline Way”: Eat a 60%-80% alkaline, immune tolerant diet (see Ten Tips for Reversing Metabolic Acidosis). Mind-body relaxation techniques, dichromatic green lights, Epsom salt and baking soda baths, abdominal breathing, and, Trager mentastics are also helpful. Water, herbal teas and fruit spritzers are beverages of choice.
Restoring tolerance and resilience to an individual’s immune function is in our experience the context for successful treatment of LD, LS and a host of other autoimmune, immune dysfunction, and inflammatory conditions.
END







